With 2017 predicted to be one of the riskiest years ever for Lyme-carrying ticks (thanks to an explosion in the mouse population last year that was thanks to a bumper crop of acorns the year before), understanding what Lyme disease is and what it looks like has never been more important. In fact, Lyme disease is severely underdiagnosed and can be an underlying challenge for many people with autoimmune disease.
Wh at Is Lyme Disease?
at Is Lyme Disease?
Chronic Lyme disease is a serious condition that the CDC reports as being the fastest growing vector-borne infectious disease (transmitted by another organism, like an insect) in the United States. Recent reports suggest that as many as 300,000 people are infected with Lyme disease every year; we are really dealing with a serious health epidemic here!
Lyme is caused by infection with the spirochete (a spiral-shaped bacteria) Borrellia burgdorferi, which has 5 subspecies and over 300 strains worldwide. This spirochete is carried by ticks and passed on to humans when an infected tick bites us. The majority of cases in the United States have been reported along the East Coast, though there have been some cases in most states. As of 2015, 95% of reported cases were isolated to 14 states in the Midwest and along the East Coast.
Ticks are small arthropods that belong to a special group of mites. Their bites break the skin, which permits the passage of infectious disease by carrier ticks (note that the percentage of ticks that are actually carrying Lyme varies between 1% and 100% depending on the region). Ticks are most likely to be found in tall grassy and woodland areas, especially during the summer months. They can be as small as a poppyseed, so many people contract Lyme disease without even being aware that they were bitten by a tick.
There’s not much that can be done to prevent contracting Lyme disease other than practicing anti-tick measures (especially in high-risk areas where the percentage of ticks carrying Lyme is particularly high), including wearing long pants in the woods and performing thorough self-checks. (There are currently no vaccines for Lyme; the most recent one, Lymerix, was taken off the market in 2002. There is one being tested but it’s several years away from being available.) For more information, the CDC has some useful tips on Preventing Tick Bites.
While the vast majority of tick bites will not result in the transmission of disease (I don’t want to scare anyone here!), it’s important to note the warning signs of an acute Lyme infection.

Signs and Symptoms of Lyme
The symptoms that occur soon after being bitten by a Lyme-infected tick are called acute Lyme disease. In some people however, symptoms can persist for months of even years after initial antibiotic treatment for Borrelia burgdorferi. And sometimes, the symptoms resolves initially but reoccur months or years later. This is typically referred to as chronic Lyme disease; however, the CDC doesn’t recognize anything beyond the initial infection (the acute phase). Much like adrenal fatigue, there are many known cases of chronic Lyme disease (and scientific studies looking at mechanisms, especially of chronic Lyme arthritis), yet functional medicine practitioners are much more likely to be trained to identify and treat chronic Lyme.
Acute Lyme Infection
There are some hallmark signs of an acute Lyme infection that merit a trip to the doctor’s office. Early signs and symptoms, occurring 3 to 20 days after a tick bite, include the following:
- Fever & chills
- Headache
- Fatigue
- Muscle and joint aches
- Swollen lymph nodes
- “Erythema migrans” rash at the site of the tick bite
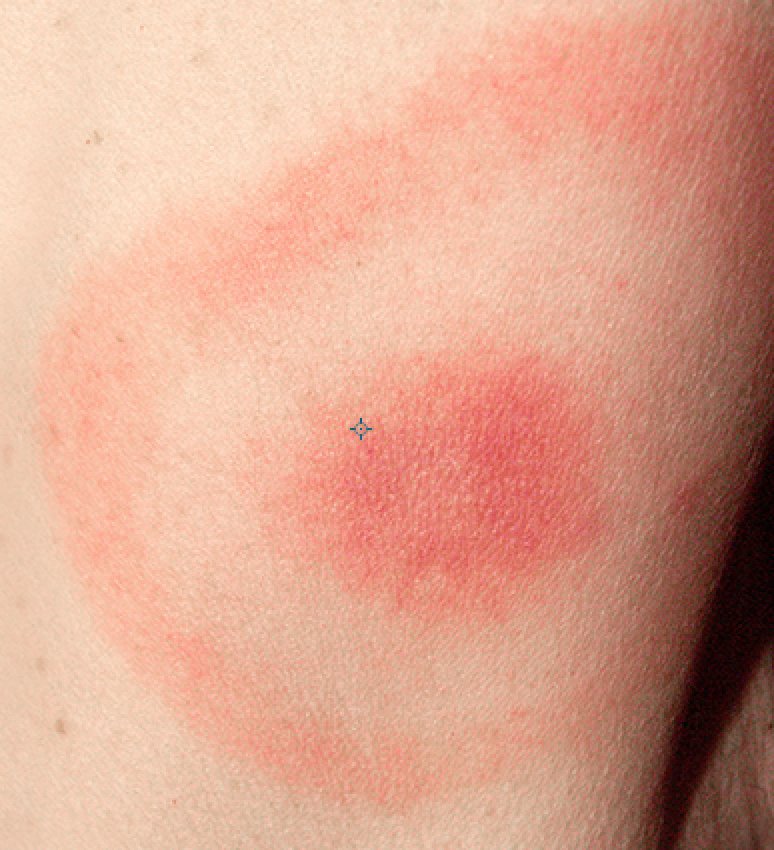 The last sign, erythema migrans, is a bullseye-like rash that starts at the site of the tick bite. The CDC states that 70-80% of reported cases feature this rash within 30 days of the bite, but there is conflicting evidence in the greater Lyme community (in fact, according to the International Lyme and Associated Disease Society, only 50% of people with chronic Lyme even recall a tick bite!).
The last sign, erythema migrans, is a bullseye-like rash that starts at the site of the tick bite. The CDC states that 70-80% of reported cases feature this rash within 30 days of the bite, but there is conflicting evidence in the greater Lyme community (in fact, according to the International Lyme and Associated Disease Society, only 50% of people with chronic Lyme even recall a tick bite!).
If the above symptoms aren’t addressed, more severe signs and symptoms may develop. These can include:
Save 70% Off the AIP Lecture Series!
Learn everything you need to know about the Autoimmune Protocol to regain your health!
I am loving this AIP course and all the information I am receiving. The amount of work you have put into this is amazing and greatly, GREATLY, appreciated. Thank you so much. Taking this course gives me the knowledge I need to understand why my body is doing what it is doing and reinforces my determination to continue along this dietary path to heal it. Invaluable!
Carmen Maier

- Severe headaches with neck stiffness
- Additional erythema migrans rashes on other areas of the body
- Arthritis with severe joint pain and swelling, especially in the knees
- Facial palsy (partial paralysis of the face)
- Intermittent pain in tendons, muscles, joints, and bones
- Heart palpitations or irregular heart beat
- Episodes of dizziness or shortness of breath
- Inflammation of the brain and spinal cord
- Nerve pain
- Shooting pains, numbness, or tingling
- Short term memory problems
These issues are no joke. If you suspect that any of the above symptoms match what you’re currently experiencing, please go to the emergency room immediately!!
Yet, it is even more complicated than this. Why? Because when Lyme disease goes untreated – and sometimes even when it is treated – people can develop a long-term, chronic form of the disease that can range from annoying to debilitating.
Chronic Lyme (AKA “Post-Treatment Lyme Disease Syndrome”)
Chronic Lyme Disease is the result of untreated or improperly treated Lyme. According to the CDC, the lingering symptoms that the alternative community have deemed chronic Lyme can be categorized “post-treatment Lyme Disease syndrome,” though there is little guidance from them about how to treat it.
Some studies report that as many as 60% of people with untreated acute Lyme disease develop chronic symptoms, most typically including joint swelling and pain (especially the knees) months or years later. And, at least 10% of those who are treated for acute Lyme will still develop chronic symptoms. Chronic Lyme disease isn’t just about joint swelling and pain however; there are many symptoms that can point to chronic Lyme disease, including:
- Fatigue
- Sleep issues
- Joint pain
- Muscle aches
- Depression
- Cognitive impairment
- Neuropathy
- Headaches
- Heart problems
There is no one course of disease when it comes to chronic Lyme. For some people, the acute Lyme symptoms persist or worsen through conventional treatment (most commonly, a very intense, weeks-long course of antibiotics); for others, the symptoms may stay dormant for a while and then resume months or years later. How is this possible? The organism that causes Lyme, Borrellia burgdorferi, is an unusual kind of bacterium that is able to evade the immune system. The theory is that Lyme spirochetes may continue to live in the host’s (infected person’s) organs, including the liver, brain, gut, and other parts of the body, and the immune system continually attacks the spirochetes. In fact, it is the immune system activation that can cause many of the symptoms associated with chronic Lyme (especially fatigue, joint pain, and brain fog).

Lyme Disease and Autoimmunity
The first indication that chronic Lyme disease might be an autoimmune disease came from a study that showed that patients with chronic treatment-resistant Lyme arthritis had a gene (HLA-DR2 and HLA-DR4) that also increases risk of rheumatoid arthritis. Other autoimmune diseases, including sarcoidosis, schizophrenia (suspected to be an autoimmune disease), and dementia (also suspected to be an autoimmune disease) have also been associated with Borrelia infections. There is evidence that Borrellia burgdorferi triggers autoimmune disease in genetically-susceptible individuals through molecular mimicry, meaning an antibody that our immune systems produce against Borrellia burgdorferi also recognizes tissues within our own bodies (antibodies against LFA-1 and CK10 have been identified as cross-reactive antibodies to Borrellia burgdorferi epitopes). And while there’s still more unknown than known, there’s ample evidence that Th1 lymphocytes are key drivers of the inflammatory response in chronic Lyme disease, another hallmark of autoimmune disease.
Chronic Lyme disease as an autoimmune disease may explain why some people with untreated acute Lyme disease suffer persistent symptoms, whereas others do not. And, it may explain why some people suffer persistent symptoms even after antibiotic treatment. If you have been diagnosed with chronic Lyme disease, it’s important to read up on the Autoimmune Protocol. While antibiotic and/or antimicrobial treatment is still indicated to eradicate the underlying infection, additional intervention (like the immune-regulating diet and lifestyle guidelines of the Autoimmune Protocol) to deal with immune activation and autoimmunity may also be required.
 Testing for Lyme Disease
Testing for Lyme Disease
For the most part, conventional doctors rely on the clinical signs and symptoms with a history of tick bite(s) to diagnose acute Lyme disease. However, there are some additional tests available. Because Lyme is known to evade the immune system, antibody tests against Lyme spirochetes may not be reliable in all people. There are some tests designed to detect the presence of whole bacteria: polymerase chain reaction (PCR), antigen detection, and culture testing. These tests are not FDA approved but may be helpful when it comes to determining the extent of Lyme infection.
Oftentimes, people with chronic Lyme disease are treated for other conditions or told by conventional physicians that they are not sick. If you suspect that you have chronic Lyme disease, working with an alternative healthcare practitioner such as a functional medicine doctor is the best option.
 Diagnosis & Next Steps
Diagnosis & Next Steps
Diagnosis will involve working with a practitioner, ideally someone in the alternative medical community who is familiar with the nuances of chronic Lyme disease, to combine your clinical picture with lab tests. Treatment for Lyme disease often involves a combination of conventional and alternative therapies (e.g., antibiotics and herbal medicine) and can take months to years to resolve, so having a community around us while going through treatment is essential.
The symptoms of chronic Lyme are often mistaken for fibromyalgia, depression, and chronic fatigue syndrome. When it comes to chronic Lyme, patients are often their own advocates.
Citations
Bockenstedt LK, Radolf JD. Xenodiagnosis for posttreatment Lyme disease syndrome: Resolving the conundrum or adding to it? Clin Infect Dis. first published online February 11, 2014 doi:10.1093/cid/cit942.
Barbour A. Remains of infection. J Clin Invest. 2012 Jul 2;122(7):2344–6. doi: 10.1172/JCI63975. Epub 2012 Jun 25.
Bockenstedt LK, Gonzalez DG, Haberman AM, Belperron AA. Spirochete antigens persist near cartilage after murine Lyme borreliosis therapy. J Clin Invest. 2012 Jul 2;122(7):2652–60. doi: 10.1172/JCI58813. Epub 2012 Jun 25.
Embers ME, Barthold SW, Borda JT, Bowers L, Doyle L, et al. (2012) Persistence of Borrelia burgdorferi in Rhesus macaques following antibiotic treatment of disseminated infection. PLoS ONE 7(1): e29914.
Feder, et al. A critical appraisal of “chronic Lyme disease”. New Eng. J. Med. 2008; 357:1422–30.Steere AC, Gross D, Meyer AL, Huber BT. Autoimmune mechanisms in antibiotic treatment-resistant lyme arthritis.J Autoimmun. 2001 May;16(3):263-8.
Kalish, RA, Leong, JM, and Steere, AC. Association of treatment-resistant chronic Lyme arthritis with HLA-DR4 and antibody reactivity to OspA and OspB of Borrelia burgdorferi. Infect Immun. 1993; 61: 2774–2779
Singh SK, Girschick HJ. Lyme borreliosis: from infection to autoimmunity. Clin Microbiol Infect. 2004 Jul;10(7):598-614.
Marques, A. Chronic Lyme disease: a review. Infect Dis Clin North Am 2008; 22:341–60.
Marques, A. et al. Xenodiagnosis to detect Borrelia burgdorferi infection: A first-in-human study. Clin Infect Dis. first published online February 11, 2014 doi:10.1093/cid/cit939.
Ghosh S, Seward R, Costello CE, Stollar BD, Huber BT. Autoantibodies from synovial lesions in chronic, antibiotic treatment-resistant Lyme arthritis bind cytokeratin-10. J Immunol. 2006 Aug 15;177(4):2486-94.
Steere AC, Falk B, Drouin EE, Baxter-Lowe LA, Hammer J, Nepom GT. Binding of outer surface protein A and human lymphocyte function-associated antigen 1 peptides to HLA-DR molecules associated with antibiotic treatment-resistant Lyme arthritis. Arthritis Rheum. 2003 Feb;48(2):534-40.





 TPV Podcast Episode 252, How Do I Lose Weight With My Restrictions Without Going Low Carb?
TPV Podcast Episode 252, How Do I Lose Weight With My Restrictions Without Going Low Carb?