 My definitive guidebook on the Autoimmune Protocol, called The Paleo Approach: Reverse Autoimmune Disease and Heal Your Body, was published way back in January of 2014. This epic tome was based on insights gleaned from over 1200 scientific studies that each illuminated a facet of the protocol.
My definitive guidebook on the Autoimmune Protocol, called The Paleo Approach: Reverse Autoimmune Disease and Heal Your Body, was published way back in January of 2014. This epic tome was based on insights gleaned from over 1200 scientific studies that each illuminated a facet of the protocol.
The benefit of basing a dietary template on scientific evidence is that it’s effective. In fact, in addition to the huge community of autoimmune disease sufferers using the AIP to mitigate their diseases, the AIP is now supported by clinical trial evidence!
In a 2017 study, fifteen patients with active inflammatory bowel disease were placed on the Autoimmune Protocol by transitioning gradually over 6 weeks, followed by a 5-week maintenance phase. Patients were closely monitored and given access to health coaching. They were also given two books, my The Paleo Approach and The Autoimmune Wellness Handbook by Mickey Trescott, NTP and Angie Alt, NTC, CHC, as resources for following the protocol. Clinical remission was achieved by week 6 (yes, just by completing the transition to the AIP) in eleven of the fifteen participants (73%!!), and they stayed in remission throughout the 5-week maintenance phase of the study. All patients, including those that didn’t achieve clinical remission, experienced quantifiable improvement in disease activity over the entire course of the study. In a similarly-designed 2019 study, seventeen women with Hashimoto’s thyroiditis were placed on the Autoimmune Protocol by transitioning gradually over 6 weeks, followed by a 4-week maintenance phase. Patients experienced a statistically significant improvement in health-related quality of life scores as measured by the 36-Item Short Form Health Survey and Cleveland Clinic Center for Functional Medicine’s Medical Symptoms Questionnaire (MSQ). In fact, the clinical symptom burden, as measured by the MSQ, decreased from an average of 92 points at the beginning of the study to 29 points after the 10 weeks. This was accompanied by statistically significant reductions in C-reactive protein (a measurement of systemic inflammation) and white blood cell counts! See also Paleo Diet Clinical Trials and Studies.
The challenge to basing a dietary template on scientific evidence is that there are limits to human knowledge. As a consequence, new scientific research has the capacity to add to our understanding of the therapeutic potential of the Autoimmune Protocol and provide valuable insight that should be integrated into the AIP framework. For this reason, it is important to periodically review the scientific literature and evaluate how it pertains to AIP guidelines and make adjustments as necessary. And, that’s exactly what I’ve done. The following updates to the AIP are the culmination of nearly three years of literature review, mainly focusing on effects of gray-area foods on immune function and gut microbiome research.
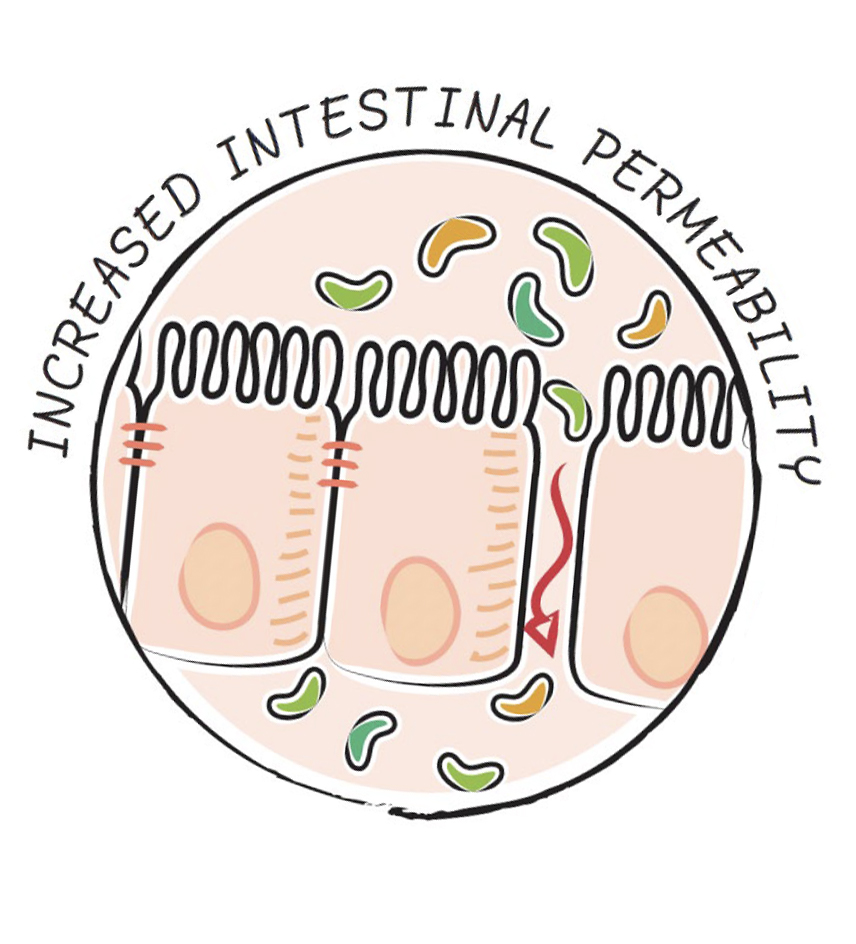 The AIP was always designed to help heal a leaky gut, with its focus on nutrients required for gut barrier health, avoiding food compounds that increase intestinal permeability, and dialing in lifestyle factors that impact the gut. Now, there’s an exciting new piece to this puzzle. Research from the last few years has shown that our gut bacteria control tight junction proteins in gut epithelial cells (enterocytes), emphasizing that we cannot restore gut barrier integrity without also supporting a healthy, diverse gut microbiome (see also What Is A Leaky Gut? (And How Can It Cause So Many Health Issues?), Which comes first: the leaky gut or the dysfunctional immune system? and What Is the Gut Microbiome? And Why Should We Care About It?). This is likely the underlying fact behind both leaky gut and gut dysbiosis being associated with every autoimmune disease in which a connection has been evaluated.
The AIP was always designed to help heal a leaky gut, with its focus on nutrients required for gut barrier health, avoiding food compounds that increase intestinal permeability, and dialing in lifestyle factors that impact the gut. Now, there’s an exciting new piece to this puzzle. Research from the last few years has shown that our gut bacteria control tight junction proteins in gut epithelial cells (enterocytes), emphasizing that we cannot restore gut barrier integrity without also supporting a healthy, diverse gut microbiome (see also What Is A Leaky Gut? (And How Can It Cause So Many Health Issues?), Which comes first: the leaky gut or the dysfunctional immune system? and What Is the Gut Microbiome? And Why Should We Care About It?). This is likely the underlying fact behind both leaky gut and gut dysbiosis being associated with every autoimmune disease in which a connection has been evaluated.
The good news is that, as I dig deep into the gut microbiome research for an upcoming new book, that the Autoimmune Protocol is already an excellent diet from a gut microbiome perspective. However, I’ve updated AIP guidelines to emphasize those foods that are especially important for supporting a healthy gut microbiome, including mushrooms (Elevating Mushrooms to Food Group Status), eating a wide variety of vegetables and fruit (ideally hitting all of the major vegetable and fruit families most days, more on this below), fish and shellfish (see Why Fish is Great for the Gut Microbiome), and polyphenol-rich foods (like extra virgin olive oil and green and black tea).
There are only a handful of foods that are known to either increase growth of key probiotic bacterial species, or improve overall composition and diversity of the gut microbiome, that are eliminated on the AIP. These include: nuts (especially walnuts, pistachios, almonds and chestnuts; see Nuts and the Paleo Diet: Moderation is Key), grass-fed A2-beta-casein dairy (like goat or sheep milk, see Goat Milk: The Benefits of A2 Dairy), chocolate, coffee (see Coffee and Autoimmune Disease), gluten-free oats, lentils, split peas, and sources of RS3 resistant starch like cooked and cooled white potatoes and white rice (see Resistant Starch: It’s Not All Sunshine and Roses). Recognizing that there’s still compelling reasons to eliminate these foods initially on the Autoimmune Protocol, but that if well-tolerated, they may have the ability to contribute to healing via benefits to the gut microbiome, it makes sense to reintroduce these foods earlier rather than later. See also Reintroducing Foods after Following the Autoimmune Protocol
Summary of Updates to the AIP
Changes to the Foods to Include:
Gut-Health Superfoods: These include high-fiber and phytonutrient fruits and vegetables, cruciferous vegetables, mushrooms, roots, tubers, alliums, leafy greens, berries, apple family, citrus, extra virgin olive oil, fish, shellfish, honey and bee products, fermented foods, edible insects, tea, and bone broth.
Changes to Suggested Order of Reintroductions
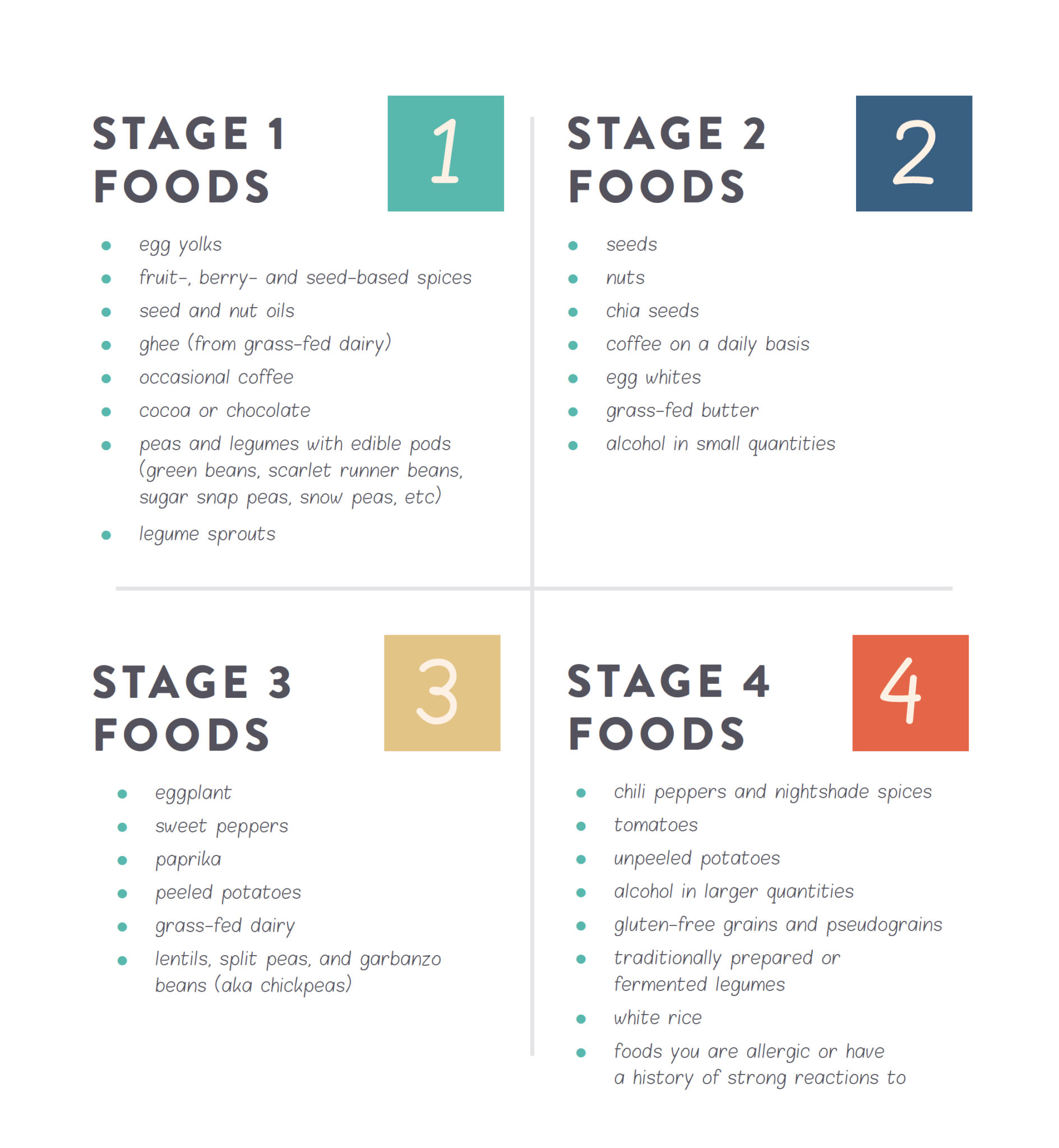
Coffee: Regular coffee consumption has been moved from Stage 3 to Stage 1 (occasional basis) and Stage 2 (daily basis).
Cocoa: Cocoa and dark chocolate (dairy-free, soy-free) has been moved from Stage 2 to Stage 1.
Save 70% Off the AIP Lecture Series!
Learn everything you need to know about the Autoimmune Protocol to regain your health!
I am loving this AIP course and all the information I am receiving. The amount of work you have put into this is amazing and greatly, GREATLY, appreciated. Thank you so much. Taking this course gives me the knowledge I need to understand why my body is doing what it is doing and reinforces my determination to continue along this dietary path to heal it. Invaluable!
Carmen Maier

Potatoes: These nightshade-family vegetables have been moved from Stage 4 to Stage 3 in peeled form, but remain in Stage 4 unpeeled.
Cashews and Pistachios: These nuts used to be in Stage 3, separated from other tree nuts and but have now moved to Stage 2 and included with other nuts and seeds.
Dairy: The highest-protein dairy products (like cheese, cottage cheese, milk, and isolates) have been moved from Stage 4 to Stage 3, with a clarification that these products be from grass-fed animals.
Legume Sprouts: Legume sprouts were not previously addressed in the reintroduction stages. They are now included in Stage 1.
Chia Seeds: Chia seeds from the other pseudograins (which remain in Stage 4) and moved them to Stage 2 with tree nuts and seeds.
Split Peas, Lentils and Garbanzo Beans: These have been separated from other dried-bean legumes (which remain in Stage 4) and moved them to Stage 3.
More Details on These Updates
Gut-Health Superfoods.

Given the strong link between gut dysbiosis and autoimmune disease, it’s also logical to emphasize gut microbiome superfoods on the AIP (along with nutrient density superstars like vegetables, organ meat, shellfish and fish). Different families of fruits and vegetables are independently beneficial for the gut microbiome, which means that hitting as many different families of vegetables and fruits per day is a very worthy goal (in addition to the goal of eating 8+ serving of veggies daily): leafy greens, cruciferous vegetables, roots and tubers (see Why Root Veggies Are Great for the Gut Microbiome), onion family, mushrooms , apple family, citrus, and berries. In fact, mushrooms get elevated to food group status thanks to their benefit to the gut microbiome (see Elevating Mushrooms to Food Group Status and The Power of Medicinal Mushrooms: An Overview).
Additionally, our gut bacteria love omega-3 fats, high-quality olive oil, fish protein (see Why Fish is Great for the Gut Microbiome), edible insects, green and black tea, honey and other bee products (see Honey: The Sweet Truth About a Functional Food!), and are also sensitive to the nutrient-density of our diet, adding yet another reason to focus on nutrient-dense foods as the foundation of our diets.
The microbiome adapts in as little as 2-3 days to big shifts in diet, so you can think of 3 days as the maximum timeframe to rotate through all gut microbiome superfoods to optimally support a healthy and diverse gut microbiome (that means mushrooms and seafood should be eaten no less frequently than once every three days). It’s also worth mentioning that our gut microbiome are also sensitive to our vitamin D levels (another reason to test for deficiency as supplement accordingly), our stress levels, our sleep, and our activity (see The Paleo Lifestyle).
There’s been a ton of new research on coffee in the last couple of years (see Coffee as a Mediator of Health & Longevity and Coffee and Autoimmune Disease). The quick summary is that coffee is anti-inflammatory is some people and inflammatory in others, and there’s still only a vague understanding of what genetics might be behind this (some autoimmune risk genes are implicated, but others aren’t, implying that coffee may help some autoimmune disease sufferers and be detrimental to others). There’s also new research showing that both fermentable substrate in coffee and antioxidants together do improve gut microbiome composition, increasing beneficial Bifidobacteria and inhibiting the growth of E. coli and Clostridium species. To reflect these two important properties of coffee, I have moved occasional consumption from Stage 2 reintroduction to Stage 1, and daily consumption from Stage 3 to Stage 2. Also see Making Healthy Choices: What’s Your Currency?
Cocoa (cacao, or dark chocolate) increases Bifidobacterium and Lactobacillus, while decreasing Bacteroides, Clostridium, and Staphylococcus species. This is thanks to cocoa’s very high polyphenol content (polyphenols are well-known modulators of gut microbiome composition, see also Polyphenols: Magic Bullet or Health Hype?). For reference, fruits and vegetables typically contain 200-300mg of polyphenols per 100g serving. A really high quality fresh-pressed olive oil may contain 300mg per quart. Dark chocolate contains a whopping 700-800mg per ounce! Interestingly, a 2016 paper used cacao polyphenols in a mouse model of autoimmune myocarditis and showed they were protective, although this needs to be viewed in the context of several studies showing that cacao polyphenols suppress Th2 and increase Th1 helper T cell activity, which may or may not be helpful depending on the details of immune function in each individual (it’s also still unclear if this effect is context dependent, meaning cocoa could be immune regulatory similar to reishi mushrooms, see The Power of Medicinal Mushrooms: An Overview, but at this point, more studies are needed to clarity cocoa’s impact on the immune system). It’s for these reasons that cocoa remains eliminated on the Autoimmune Protocol but moves from a Stage 2 reintroduction to a Stage 1. Also see Making Healthy Choices: What’s Your Currency?
Grass-Fed Dairy (Preferably A2).
 Grass-fed dairy is a very rich source of conjugated linoleic acid, linked with reduced risk of cardiovascular disease, obesity, cancer, diabetes, osteoporosis and lower levels of inflammation (see Conjugated Linoleic Acid (CLA): A Rockstar Nutrient and Goat Milk: The Benefits of A2 Dairy). This may be mediated through CLA’s benefits to gut microbiome composition, as it is also known to have a prebiotic effect on Bacteroidetes/Prevotella and Akkermansia muciniphila. In addition, A2 beta-casein is not associated with the skewing of the gut microbiome nor the increase in gastrointestinal inflammation (including Th2 cell activation) that A1 beta-casein is. It is certainly preferable for autoimmune disease sufferers to stick to grass-fed A2 dairy (A2 cows, goat, sheep, etc.). With this caveat however, if butter is well-tolerated in Stage 2 reintroductions, methodical reintroduction of other dairy products (from the same animal) can all be undertaken in Stage 3.
Grass-fed dairy is a very rich source of conjugated linoleic acid, linked with reduced risk of cardiovascular disease, obesity, cancer, diabetes, osteoporosis and lower levels of inflammation (see Conjugated Linoleic Acid (CLA): A Rockstar Nutrient and Goat Milk: The Benefits of A2 Dairy). This may be mediated through CLA’s benefits to gut microbiome composition, as it is also known to have a prebiotic effect on Bacteroidetes/Prevotella and Akkermansia muciniphila. In addition, A2 beta-casein is not associated with the skewing of the gut microbiome nor the increase in gastrointestinal inflammation (including Th2 cell activation) that A1 beta-casein is. It is certainly preferable for autoimmune disease sufferers to stick to grass-fed A2 dairy (A2 cows, goat, sheep, etc.). With this caveat however, if butter is well-tolerated in Stage 2 reintroductions, methodical reintroduction of other dairy products (from the same animal) can all be undertaken in Stage 3.
White potatoes, especially when cooked and then cooled (and reheated, if eating warm is desired), are an excellent source of RS3 resistant starch, a boon to the gut microbiome (see What is a “Safe Starch”? and Resistant Starch: It’s Not All Sunshine and Roses. Given that glycoalkaloids are typically concentrated in the peel of the potato, it makes sense to try reintroducing peeled potatoes a little sooner, which is why peeled potatoes have moved from Stage 4 to Stage 3. You can read about the glycoalkaloid levels in peel versus flesh of different varieties of potatoes in Potatoes: Friend or Foe of Paleo?
Pistachios and Cashews.
 Pistachios are well-known to be extremely beneficial for the gut microbiome, above and beyond almonds and chestnuts, and almost as much as walnuts. (There is a dearth of data on other nuts and the gut microbiome, but it can be expected that highly related nuts would have similar effects.) It is for this reason that they’ve been combined with other nuts and seeds as Stage 2 reintroductions, although anyone with severe poison ivy reactions or allergies to mango should exercise caution when reintroducing pistachios and cashews. See also Nuts and the Paleo Diet: Moderation is Key
Pistachios are well-known to be extremely beneficial for the gut microbiome, above and beyond almonds and chestnuts, and almost as much as walnuts. (There is a dearth of data on other nuts and the gut microbiome, but it can be expected that highly related nuts would have similar effects.) It is for this reason that they’ve been combined with other nuts and seeds as Stage 2 reintroductions, although anyone with severe poison ivy reactions or allergies to mango should exercise caution when reintroducing pistachios and cashews. See also Nuts and the Paleo Diet: Moderation is Key
Legume Sprouts. I have always viewed legume sprouts (such as mung bean sprouts) as a gray area, classifying them similarly to legumes with edible pods. They contain only a fraction of the phytates and agglutinins that dried beans do, and what they do contain is much more easily deactivated by heat. Frequent questions from the AIP community necessitated adding them to the reintroduction stages. See also The Green Bean Controversy and Pea-Gate
The pseudograins buckwheat, amaranth and quinoa are all rich in problematic compounds, including saponins and amylase-trypsin inhibitors, and the prolamins in both quinoa and amaranth are known gluten cross-reactors. Chia may be a different story however. It comes from a different family than quinoa, buckwheat or amaranth and chia doesn’t appear to contain the problematic compounds identified in other pseudograins. In fact, the only reason chia isn’t being incorporated into the elimination phase of the AIP is the lack of information currently available about the impact of its high mucilage fiber content. While mucilage tends to be beneficial for the gut microbiome, it also modulates the immune system in complex and potentially detrimental ways for anyone with autoimmune disease. In particular, some types of mucilage specifically stimulate either the Th1 immune response (like flaxseed) or the Th2 immune response (like natto). Because there are many unanswered questions about the impact of chia mucilage on immune function, it is initially eliminated on the AIP. See also Are Pseudograins Pseudobad? and Mucilaginous Fiber: The Good, the Bad, and the Gooey
 Peas, Lentils and Garbanzo Beans.
Peas, Lentils and Garbanzo Beans.
Peas, lentils and garbanzo beans are especially beneficial for the gut microbiome while containing lower amounts of antinutrients and agglutinins that are more easily deactivated by heat than other legumes like kidney beans, soy, and peanuts. For this reason, it seemed prudent to separate them from other legumes and encourage reintroduction earlier than previously. See also The Green Bean Controversy and Pea-Gate
Both pea protein and pea fiber are beneficial for the gut microbiome. Pea protein has been shown to increase levels of important short-chain fatty acids in the intestine, indicating that it feeds SCFA-producing bacteria in the gut. In a rat study comparing the effects of different legumes in diets with equal protein and calorie levels, pea consumption resulted in higher counts of Bifidobacterium than any other legume tested. This has been confirmed in humans, with pea protein significantly increasing levels of beneficial Lactobacillus, Bifidobacterium and Enterococcus while suppressing Escherichia. Pea fiber increases abundance of Lachnospiraceae and Prevotellaceae and shifts the microbiome to a phenotype responsible for better glucose tolerance. In addition, the changes in the microbiome that result from pea fiber supplementation coincide with increased expression of genes relating to gut barrier health.
Lentils increase abundance of probiotic strains of Actinobacteria and Bacteroidetes, while increasing resistance to pathogen colonization in the gut. The microbiome changes resulting from high lentil consumption are also associated with leanness and lower cardiovascular disease risk factors.
Garbanzo bean fiber increases levels of Bifidobacterium and Lactobacillus in addition to promoting the secretion of SCFAs (especially propionate and butyrate).Garbanzo bean fiber (at least in mice) can even protect against the dysbiosis caused by high-fat diets.
Need More Info?
If reading this post makes you hungry for more information on the AIP or for a more detailed explanation of the science above, consider registering for the next session of The AIP Lecture Series!
The Autoimmune Protocol Lecture Series is a 6-week video-based, self-directed intensive online course that will teach you the scientific foundation for the diet and lifestyle tenets of the Autoimmune Protocol, plus provide tons of tips and strategies for implementation, refinement, reintroductions and troubleshooting!
The AIP Lecture Series is the ultimate Autoimmune Protocol educational experience! You’ll learn directly from me, with 42 on-demand video lectures, dozens of printables guides, daily self-discovery exercises, interactive quizzes and even an online forum to connect with me, join group discussions, ask your questions and get personalized guidance and support!










 Eggplant and Wild Mushroom Stuffing
Eggplant and Wild Mushroom Stuffing