In the Paleo community, the idea of taking antibiotics is often frowned upon, and it’s easy to see why! A huge body of research shows that antibiotics not only destroy beneficial bacteria while they’re being taken, but also alter the gut microbiome in ways that can be irreversible. In other words, it’s not always possible to fully restore the diversity of microbes we originally had after we’ve taken a round (or several!) of antibiotics. (Not to mention, they can cause some seriously unpleasant side effects—like diarrhea, rashes, nausea, vomiting, dizziness, headache, taste alteration, abdominal pain, lethargy, and insomnia… just to name a few!) Plus, overusing antibiotics can result in resistant strains that no longer respond to drug therapy, leading to infections that are much harder to treat (like MRSA).
Table of Contents[Hide][Show]
Depressing, right? So, it’s no surprise that many of us want to avoid antibiotics altogether and find less intrusive ways to heal!
But, that doesn’t change the fact that, in some situations, antibiotics are absolutely needed. It’s definitely smart to avoid antibiotics when they aren’t really necessary (like viral flus and colds), but when it comes to certain illnesses and infections (the ones that used to wipe out huge chunks of the human population!), antibiotics can prevent serious complications and even save our lives. There’s no reason we should ever feel guilty or like we’ve “failed” just because we need to take antibiotics. While following the Paleo diet typically supports much stronger and well-regulated immune systems, it does not (sadly) make us invisible. The necessity for antibiotics doesn’t mean that you didn’t “Paleo hard enough” so don’t be hard on yourself. And while it’s always a good idea to reflect on ways that we can improve the quality and consistency of our diet and lifestyle choices, what’s most important while recovering from illness is making science-based, informed choices that give us the best chance of getting healthy efficiently!
Fortunately, by understanding how antibiotics affect our health and what we can do to combat their unpleasant effects, we can take steps to minimize the damage and restore our health as quickly as possible.
Save 80% Off the Foundations of Health
Expand your health knowledge on a wide range of topics relevant to you, from how to evaluate scientific studies, to therapeutic diet and lifestyle, to leaky gut and gut microbiome health, to sustainable weight loss, and much more!!!

What Are Antibiotics?
 The word antibiotic literally means “against life” from its Greek roots. And, that’s exactly what this form of medicine is designed to do: antibiotics stop or slow down the growth of microscopic organisms (bacteria, fungi, and some parasites), in turn treating potentially dangerous infections.
The word antibiotic literally means “against life” from its Greek roots. And, that’s exactly what this form of medicine is designed to do: antibiotics stop or slow down the growth of microscopic organisms (bacteria, fungi, and some parasites), in turn treating potentially dangerous infections.
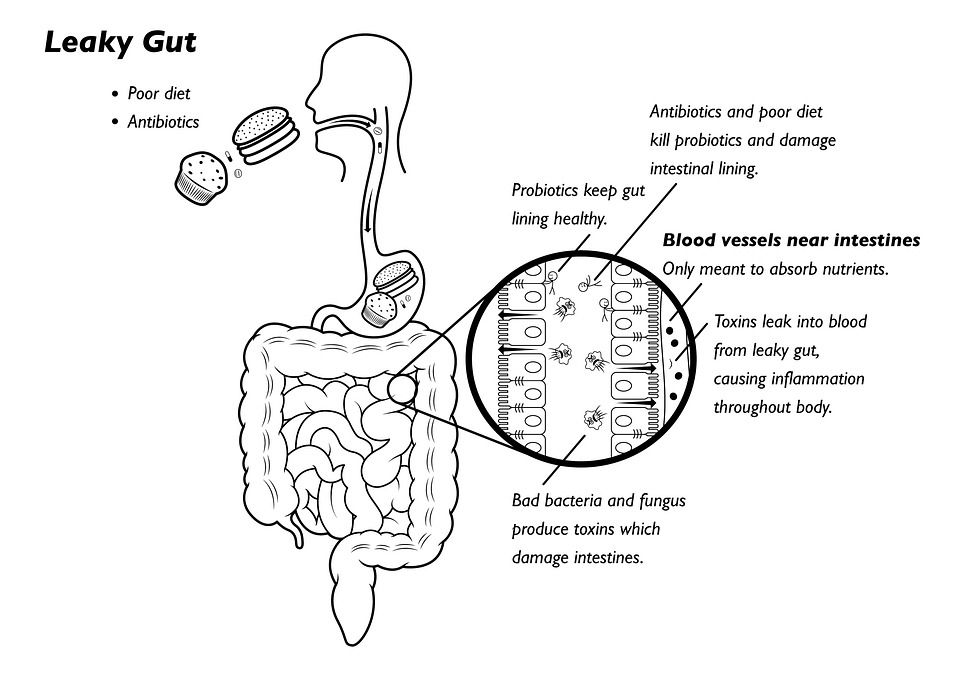
The problem is, in the process of wiping out “bad” microbes, antibiotics can also destroy beneficial bacteria and yeast that mediate an incredible array of processes in our body (like maintaining gut barrier integrity, tuning the immune system, and increasing bioavailability of nutrients from our food)! We want those good microbes to stay diverse and abundant in order to support our health. So, whenever we embark on antibiotic therapy, the goal should be to protect, preserve, and restore these beneficial organisms as much/soon as possible.
What to Do While Taking Antibiotics
There’s a common belief that we should wait until we’ve finished a course of antibiotics before trying to rebuild our gut flora with probiotics (either because the probiotics will interfere with the antibiotics’ effectiveness, or because they’ll just been rendered useless). Actually, this is a total misconception! Taking probiotics during antibiotic therapy is one of the most helpful things we can do for maintaining gut health.
How does it work? Both during and after antibiotic therapy, probiotics can help by stimulating immunity, producing antimicrobial substances, competing for receptors and nutrients that pathogens are also trying to get, inhibiting harmful bacteria from adhering to the gut lining, and even lowering the pH of the colon (which helps nonpathogenic bacteria bloom, instead of the bad guys!). Even if the probiotics we ingest during antibiotic therapy don’t take up permanent residence yet, they can still help keep pathogens at bay and prevent crazy microflora imbalances.
A number of studies have examined the effects of probiotics on antibiotic-induced side effects, and the results have been impressive! It turns out that probiotics can go a long way to reduce unpleasant symptoms, especially gastrointestinal distress like diarrhea (which can occur when antibiotics wipe out the competitors for pathogenic bacteria and allow diarrhea-inducing strains to flourish). One meta-analysis looked at 63 trials on probiotics for preventing antibiotic-associated diarrhea (among people being treated for Clostridium difficile infections), and found a major reduction in diarrhea occurrence when people took Lactobacillus-based probiotics (a relative risk of 0.58 for people being treated with probiotics during antibiotic therapy). Other meta-analyses found that Saccharomyces boulardii and Lactobacillus rhamnos, in particular, were very helpful for reducing antibiotic-associated diarrhea. And, additional studies have found various probiotic strains (especially Lactobacillus) can help reduce nausea, taste disturbance, headaches, hypersensitivity, and other symptoms when taken during a round of antibiotics!
One study actually tested the effects of starting probiotics (Lactobacillus acidophilus and Bifidobacterium bifidum) after antibiotic therapy versus during antibiotic therapy (and continuing for a week after the antibiotic course was completed). The group that started taking probiotics while still on antibiotics had more stable levels of microflora and less gut dysbiosis throughout the experiment!
So, what does this mean for us? Although different trials have successfully used different strains and quantities of probiotics, these are the major takeaways:
 Load up on fermented foods teeming with natural probiotics! These include raw, unpasteurized sauerkraut, kimchi, fermented carrots, fermented beets, pickles, fermented fruits (chutneys, jams, pickled jackfruit, green papaya), kombucha, beet kvass, coconut milk kefir, coconut milk yogurt, and raw condiments (like “real” ketchup, salsas, pickled ginger, and relishes). For people who aren’t sensitive to dairy or soy, unpasteurized yogurt and kefir, natto, miso, tempeh, and tamari sauce are also great options. For the best results, eat these foods 2 to 4 hours after an antibiotic dose.
Load up on fermented foods teeming with natural probiotics! These include raw, unpasteurized sauerkraut, kimchi, fermented carrots, fermented beets, pickles, fermented fruits (chutneys, jams, pickled jackfruit, green papaya), kombucha, beet kvass, coconut milk kefir, coconut milk yogurt, and raw condiments (like “real” ketchup, salsas, pickled ginger, and relishes). For people who aren’t sensitive to dairy or soy, unpasteurized yogurt and kefir, natto, miso, tempeh, and tamari sauce are also great options. For the best results, eat these foods 2 to 4 hours after an antibiotic dose.- Take probiotic supplements (especially if you’re yeast or histamine sensitive or otherwise don’t do well with fermented foods!). For preventing antibiotic-associated diarrhea and other side effects, an intake of at least 5 billion CFU/day for children or 10 billion CFU/day per adults is recommended (up to 40 billion CFU/day may be optimal in some cases). A number of existing trials show that Lactobacilli, Bifidobacteria, and Saccharomyces boulardii are the most effective types for reducing antibiotic side effects. All probiotics should be consumed with food, and bacterial strains should be taken at least 2 to 4 hours after each antibiotic dose (so that they don’t get inhibited by the antibiotic itself). (For more info on my probiotic recommendations, check out this post!)
- Focus on yeast! Saccharomyces boulardii is actually a form of probiotic (yes, beneficial!) yeast, which makes it particularly useful while taking bacteria-killing antibiotics, because it won’t be destroyed. Consuming 250–1000 mg daily during the course of antibiotic therapy is a common recommendation.
- Consume plenty of bone broth (or other sources of glycine, like gelatin) to help maintain the integrity of the gut lining, since the shift in microbial proportions from antibiotics can increase the risk of leaky gut.
What to Do After Taking Antibiotics
Once we’ve completed antibiotic therapy, it’s time to seriously buckle down and get our gut microbiome back in shape! Chances are, the antibiotics caused a major loss in microbial diversity, wiped out a number of beneficial species, and may have allowed pathogenic strains to flourish. So, the goal now is to rebalance the microbiome and restore as much (good) diversity as possible!
 Continue eating plenty of raw, unpasteurized, fermented foods throughout the day. Because these typically contain a huge spectrum of probiotic species, they offer greater microbial diversity than most probiotic supplements. Lacto-fermented fruits, vegetables, and beverages tend to be high in Lactobacillus and Bifidobacteria, while kefir and kombucha are great sources of Saccharomyces boulardii. Eat from as many categories of fermented foods as possible to get a variety of awesome microbes, both bacterial and yeast!
Continue eating plenty of raw, unpasteurized, fermented foods throughout the day. Because these typically contain a huge spectrum of probiotic species, they offer greater microbial diversity than most probiotic supplements. Lacto-fermented fruits, vegetables, and beverages tend to be high in Lactobacillus and Bifidobacteria, while kefir and kombucha are great sources of Saccharomyces boulardii. Eat from as many categories of fermented foods as possible to get a variety of awesome microbes, both bacterial and yeast!- Continue to take a minimum of 10 billion CFUs of probiotics daily for at least 3 weeks after the antibiotic therapy has ended. Even after discontinuing antibiotics, there’s still a risk of developing antibiotic-associated diarrhea, and focusing on key varieties (Lactobacillus, Bifidobacteria, and Saccharomyces boulardii) will help prevent potential gastrointestinal side effects.
- Load up on a variety of prebiotic-rich plant foods! These include leafy greens, root veggies, plantains, bananas, taro, cassava, garlic, Jerusalem artichokes, chicory roots, and onions, which provide an array of prebiotic fibers and resistant starches (excellent food for beneficial microbes). Although some people recommend taking isolated resistant starch as a prebiotic supplement, I strongly encourage using only whole-food sources (check out this post to learn why!).

Then What?
In the weeks and months following antibiotic treatment, these protocols should help restore a great deal of microbial diversity and abundance in our guts. But, maintaining a healthy gut should be a long-term priority. And the unfortunate reality is, we’re exposed to a ton of diet and lifestyle factors that harm our microbiomes, regardless of whether we’ve taken antibiotics or not. Stress, lack of sleep, sedentary living, certain medications, and a poor diet (among many other things!) can all negatively impact our gut flora and increase the risk of dysbiosis. What to do?! Our best bet is to eat a nutrient-dense Paleo diet rich in prebiotic and probiotic components (tons of veggies aiming for at least 40g of fiber daily and incorporating fermented foods), go to bed at a decent hour (this is a fantastic resource), stay physically active (see here), and take measures to eliminate or better handle the stress in our lives. Not only will our immune systems be stronger (and better able to ward off infection in the first place), but if a time comes when we do need antibiotics, our bodies will be much better equipped to handle the aftermath.
Citations
Ambrose NS, et al. “The influence of single dose intravenous antibiotics on faecal flora and emergence of Clostridium difficile.” J Antimicrob Chemother. 1985 Mar;15(3):319-26.
Armuzzi A, et al. “The effect of oral administration of Lactobacillus GG on antibiotic-associated gastrointestinal side-effects during Helicobacter pylori eradication therapy.” Aliment Pharmacol Ther. 2001 Feb;15(2):163-9.
Cremonini F, et al. “Probiotics in antibiotic-associated diarrhoea.” Dig Liver Dis. 2002 Sep;34 Suppl 2:S78-80.
D’Souza AL, et al. “Probiotics in prevention of antibiotic associated diarrhoea: meta-analysis.” BMJ. 2002 Jun 8;324(7350):1361.
Hempel S, et al. “Probiotics for the prevention and treatment of antibiotic-associated diarrhea: a systematic review and meta-analysis.” JAMA. 2012 May 9;307(18):1959-69.
Hickson M, et al. “Use of probiotic Lactobacillus preparation to prevent diarrhoea associated with antibiotics: randomised double blind placebo controlled trial.” BMJ. 2007 Jul 14;335(7610):80.
Janeway CA Jr, et al. “Immunobiology: The Immune System in Health and Disease. 5th edition.” New York: Garland Science; 2001.
Jones K. “Probiotics: preventing antibiotic-associated diarrhea.” J Spec Pediatr Nurs. 2010 Apr;15(2):160-2.
Kliger B & Cohrssen A. “Probiotics.” American Family Physician. 2008 Nov 1;78(9):1073-1078.
Koning CJ, et al. “The effect of a multispecies probiotic on the intestinal microbiota and bowel movements in healthy volunteers taking the antibiotic amoxycillin.” Am J Gastroenterol. 2008 Jan;103(1):178-89.
Madden JA, et al. “Effect of probiotics on preventing disruption of the intestinal microflora following antibiotic therapy: a double-blind, placebo-controlled pilot study.” Int Immunopharmacol. 2005 Jun;5(6):1091-7.
McFarland LV. “Meta-analysis of probiotics for the prevention of antibiotic associated diarrhea and the treatment of Clostridium difficile disease.” Am J Gastroenterol. 2006 Apr;101(4):812-22.
Rolfe RD. “The role of probiotic cultures in the control of gastrointestinal health.” J Nutr. 2000 Feb;130(2S Suppl):396S-402S.
Szajewska H & Mrukowicz J. “Meta-analysis: non-pathogenic yeast Saccharomyces boulardii in the prevention of antibiotic-associated diarrhoea.” Aliment Pharmacol Ther. 2005 Sep 1;22(5):365-72.
Vanderhoof JA, et al. “Lactobacillus GG in the prevention of antibiotic-associated diarrhea in children.” J Pediatr. 1999 Nov;135(5):564-8.
Verdú EF, et al. “Specific probiotic therapy attenuates antibiotic induced visceral hypersensitivity in mice.” Gut. 2006 Feb;55(2):182-90. Epub 2005 Aug 16.



 TPV Podcast, Episode 191, Help, I resent my diet!
TPV Podcast, Episode 191, Help, I resent my diet!