Chronic stress can lead to adrenal fatigue, a condition in which the adrenal glands cease to function properly, and characterized by a collection of symptoms, which can include: fatigue, poor sleep or insomnia, mood swings, unexplained weight gain or loss, inflammation, high cardiovascular disease risk factors, insulin resistance, decreased sex drive, joint pain, and frequent infections like colds and flu (see Demystifying Adrenal Fatigue, Pt. 1: What is Adrenal Fatigue?).
Table of Contents[Hide][Show]
Proper testing is critical for diagnosis, especially considering the number of common conditions that can be confused with adrenal fatigue, and for determining the appropriate route of treatment (Demystifying Adrenal Fatigue, Pt 2: Testing Adrenal Glandular Function).
Now, we get to go through the more practical information: specific ways to support adrenal glandular function. All of the recommendations below are naturally-oriented but scientifically-backed, gentle methods to support these critical organs. Keep in mind that none of these strategies replace the medical expertise of a practitioner! If adrenal fatigue is suspected, the best course of action is to seek out someone qualified to order and interpret the tests described in Part 2. The good news is that there are many ways we can support healthy adrenal glands!
Nutrition for Adrenal Support
The very specific nutritional strategies for someone in stage 2 or 3 adrenal fatigue are going to depend on each very specific case, so we won’t go into meal-planning-level detail here. But, based on the science of adrenal gland function and cortisol secretion, there are three easy ways that we can support our adrenal glands regardless of their status.
Save 80% Off the Foundations of Health
Expand your health knowledge on a wide range of topics relevant to you, from how to evaluate scientific studies, to therapeutic diet and lifestyle, to leaky gut and gut microbiome health, to sustainable weight loss, and much more!!!

Eat an Anti-Inflammatory Diet!
 One of the main functions of cortisol is to act as an immune suppressor (see Demystifying Adrenal Fatigue, Pt. 1: What is Adrenal Fatigue?). When we have elevated systemic inflammation, which is the baseline level of immune system activity in the body, our adrenal glands secrete more cortisol in order to attempt to control the inflammation. If we work to reduce our systemic inflammation, our bodies will release less cortisol overall, regardless of the amount of chronic stress we’re experiencing (but we’ll be discussing that more later!!).
One of the main functions of cortisol is to act as an immune suppressor (see Demystifying Adrenal Fatigue, Pt. 1: What is Adrenal Fatigue?). When we have elevated systemic inflammation, which is the baseline level of immune system activity in the body, our adrenal glands secrete more cortisol in order to attempt to control the inflammation. If we work to reduce our systemic inflammation, our bodies will release less cortisol overall, regardless of the amount of chronic stress we’re experiencing (but we’ll be discussing that more later!!).
So, how do we control inflammation? Implementing a Paleo diet, or better yet a Paleo Autoimmune Protocol, that emphasizes anti-inflammatory foods is the very best way to control diet-related systemic inflammation. The Paleo diet is an evidence-based series of dietary recommendations that encourages the elimination of grains, dairy, legumes, refined oils, processed sweeteners and additives (i.e., preservatives, artificial sweeteners, artificial coloring, etc.) while simultaneously increasing consumption of the most nutrient-dense options like seafood, organ mean, and a huge variety of vegetables (see The Importance of Nutrient Density and The Diet We’re Meant to Eat, Part 3: How Much Meat versus Veggies?). Clinical trials demonstrate that a Paleo diet improves cardiovascular disease risk factors, reduces inflammation, improves glucose tolerance, helps with weight loss, lowers colon cancer risk, and can even improve autoimmune disease (see Paleo Diet Clinical Trials and Studies).
However, when focusing on trying to reduce our systemic inflammation, we might need to be a little extra cautious and stricter when it comes to our Paleo template. For example, grains are known to be particularly inflammatory, especially gluten-containing grains (i.e., wheat, barley). So, even if we believe that gluten doesn’t cause a reaction for us, taking a break from gluten-full grains might be a good idea until the adrenal concerns are under control.
Apart from being strict about a Paleo protocol, there are specific nutrients that we can focus on: namely, getting the right kind of fatty acids! Omega-3 fatty acids are known to help prevent and reduce inflammation, with positive outcomes including lowering cardiovascular disease risk. And, new research has specifically linked omega-3 intake with better sleep. Just another reason to get your fatty, coldwater fish intake up! Omega-6 and omega-3 fatty acids directly compete for space in your cellular membranes (which is where they’re stored and then used to either fight infection or reduce inflammation), so knowing about how much you’re eating of each could be huge for promoting an anti-inflammatory lifestyle (see Why Grains Are Bad, Part 2: Omega 3 vs. 6 Fats and Which Fats Should You Eat?). Try to increase your omega-3 intake by eating more wild-caught fish (canned salmon and sardines are great, inexpensive options), omega-3 eggs, and maybe also using a fish oil supplement (good for short-term use only, think 4-6 weeks). Similarly, it is also important to reduce our intake of omega-6 fatty acids to the best of our ability (and budget). Omega-6 fatty acids would most commonly be found in poultry, nuts, seeds, eggs, and avocado in our Paleo template; outside of the Paleo world, you’d find a boatload of omega-6s in cereals, whole grain breads, and vegetable oils.
 Avoid Xenohormones
Avoid Xenohormones
There are some additional basic strategies that promote adrenal gland health regardless of whether we have suspected adrenal fatigue. As we discussed in Part 1, the adrenal glands are hugely responsible for hormonal balance in the body, and there are complicated pathways that lead to cholesterol being converted to a variety of hormones, including cortisol, estrogen, and progesterone. One way that we can support our adrenal glands is to reduce the amount of xenohormones that we consume or are otherwise exposed to.
Xenohormones are any kind of external hormone analog (a chemical compound that resembles a hormone that is not created by the human body). There are a shocking number of sources of xenohormones in the modern world. Why do we want to limit our consumption and/or exposure to them? It’s simple: adding exogenous hormones to the adrenal gland cycle could drastically impact the hormonal pathways for which the adrenal glands are responsible, offsetting the HPA or HPG axes that we discussed in Part 1. And, as we know, a disruption in these axes can contribute to adrenal fatigue (and other problems, such as unexplained weight loss or gain, thyroid problems, and reproductive problems).
Phytoestrogens are the estrogen analogs found in many plants, especially legumes. In fact, this is one of the reasons that legumes are generally excluded from the Paleo diet: this group of plants, especially soy, are rich in a series of phytoestrogens that can be hugely disruptive to our hormonal regulation!! Other sources of phytoestrogens include flax seeds, sesame seeds, walnuts, and pretty much any processed food.
There are other sources of exogenous hormones that are noteworthy here. It’s important to remember that the animals we eat also produce hormones that may act as xenohormones as well. Animals that are fed a diet that includes synthetic hormones could be particularly problematic; those excess hormones force them to grow quickly (yet another reason to opt for humanely-raised meat) but also means their meat contains more hormones that can affect our health. Compounds from certain pesticides, plastics, and detergents also act as hormones in the body.
One simple way to avoid this problem is to go organic (or find a local farm that utilizes organic practices but may not be able to get the expensive certification). If we can get our hands on organic, humanely-raised, grass-fed or pastured meat, it is richer in omega-3 fatty acids, too! While it can be more expensive to prioritize these types of meat, seafood, and produce, it might be an essential way to combat adrenal problems and hormonal imbalance (both from a preventative perspective and a potential therapeutic perspective).
And, just one more set of bad news: a lot of conventional body products also have additives that can act as xenohormones. And in the case of things like makeup, we don’t always get a clear label that includes what the makeup is made of! When it comes to body care products, it’s no secret that I love Morrocco Method for “shampoo,” Primal Life Organics and Buffalo Gall Grassfed Beauty for skincare, and Araza (100% natural and Paleo!) for makeup.
 Cut Out Coffee
Cut Out Coffee
And now, we come to what might be the toughest option out of all of these: reducing or eliminating coffee. Anyone who’s been following me for a long time knows that I just simply love the taste of coffee. I gave it up for 15 months when I adopted the Autoimmune Protocol, and it wasn’t easy to live without! The thing is, coffee is a known stimulant of the immune system and adrenal glands; consuming coffee leads to an increase in our daily release of cortisol and is known to increase psychological symptoms such as anxiety (and that in of itself can increase cortisol release, too! see The Pros and Cons of Coffee).
When we consume caffeine, our cortisol level increases (though it’s noteworthy that this depends on what our cortisol management looks like to begin with and how much caffeine we consume) and can stay elevated for up to 6 hours. With daily consumption, our bodies adapt somewhat and will not produce quite as much cortisol, but complete tolerance to caffeine does not occur. Very importantly, if we habitually consume caffeine, our cortisol will increase more dramatically in response to stress (like that guy cutting you off in traffic) than someone who doesn’t consume caffeine. If you have difficult managing stress as it is, caffeine is not particularly helpful.
One key study showed that moderate coffee consumption in healthy individuals correlated with increased markers of inflammation in their blood (that would be the systemic inflammation we’ve been discussing). People who drank more than 200mL (that’s one large cup in my house) of coffee every day (equivalent to 37.3mg of caffeine, which frankly is not that much – the FDA recommended maximum dose for pregnant women is 200mg! Just for some context) had increased circulating white blood cells and several key inflammatory cytokines (chemical messengers of inflammation, usually restricted to the site of injury or infection). When cytokines circulate in the blood, they cause low level inflammation everywhere in the body. This chronic systemic inflammation is exactly one of the situations we are trying to prevent with adoption of a Paleo diet and attempting to prevent or combat adrenal fatigue! These increases in markers of inflammation were persistent even after adjusting for other health and lifestyle factors (such as age, sex, weight, exercise, and smoking). While we know that there is a lot of variation in how everyone responds to stress and caffeine consumption, it’s important to take studies like this into consideration.
Another factor to think about is whether your genetics contribute to the way you metabolize caffeine. I know, that sounds kind of crazy, but we actually know which genes contribute to caffeine metabolism in the liver (everything goes through a complicated detoxification pathway regulated by a series of proteins are encoded for by the p450 genes). The function of these genes determines how much of an effect we feel from caffeine and how long it continues to act in the body. So, fast metabolizers are more likely to feel the effect of caffeine quickly and have their livers process and remove it quickly as well. On the other hand, slow metabolizers process and remove it much more slowly, so they may feel less effects but for longer (sometimes up to 12 hours, actually – an important thing to consider when thinking about sleep-wake cycles, too!).
Interested in cutting caffeine out of your life? I highly suggest weaning off of coffee rather than trying to go cold turkey; the withdrawal process can be really brutal for daily users. Substituting for black tea is another option that tends to be less harsh on people. There are also completely non-caffeinated options, like roasted chicory “coffee.”
Lifestyle for Adrenal Support
Supporting the adrenal glands goes way beyond nutrition. In fact, improving adrenal gland function really requires a lifestyle overhaul. Luckily, there are several lifestyle factors that we can tweak to support the adrenal glands.
 Choose Gentle Exercise
Choose Gentle Exercise
Some of us are big fans of intense exercise, but the unfortunate reality is that vigorous workouts (cough cough, CrossFit, cough cough) result in a spike in the release of cortisol. However, if you keep exercise to a more appropriate duration and intensity for your fitness level (and appropriate for how well you eat, sleep and manage stress in other areas of your life), exercise becomes very potent at reducing and normalizing cortisol levels (which can also help reduce inflammation and promote healing). This makes it easier to burn stored energy (especially fat), improves your sleep, and makes you feel more relaxed and able to cope with life’s surprises.
While exercise has tons of benefits, like reducing our risk of heart disease, certain cancers, diabetes, insulin resistance, stress, anxiety, cognitive decline, and a host of other things we all want to avoid, even gentle movement like a slow amble has tremendous benefits (see The Benefits of Gentle Movement)! Our society focuses a lot on the act of going to the gym to “pay off” a caloric debt for all of the “bad” foods we eat and the time we spend at work desks. Elsewhere in the world, we can see more realistic models of what the human body is adapted to in terms of daily movement. Ethnographic accounts of hunter-gatherers show that both men and women participated in regular movement to keep their societies running smoothly. Men were often in charge of hunting large game, trekking long distances and mixing periods of rest with spikes of brief, intense exertion. In many tribes, women were in charge of foraging for edible plants and small animals or eggs—with periods of rest interspersed with hours of walking, digging, stretching, and bending in order to collect food and bring it back to camp. Hunter-gatherer mothers also had to carry their children around through infancy and toddlerhood, and by some estimates, would walk nearly 3,000 miles with a child in their arms during the child’s first four years of life. As anyone with children knows, that’s no easy feat!
I recommend setting a timer to go off every 20 minutes during your day. Along with interrupting sedentary periods with movement breaks, you can also try being in a constant (or near-constant) state of gentle movement throughout the day. Clearly, the treadmill desk is a great option for this, but it’s not the only one! One great way to increase movement while sitting is getting a cheap and inconspicuous DeskCycle, which is just the pedals and gears of a stationary bike. You can slide it under your desk at work or at home and engage in some gentle movement without distracting the people around you.
 Get Good Sleep
Get Good Sleep
Getting adequate quality sleep is probably the single most important thing that we can do for adrenal health. A growing number of studies show that poor quality sleep or chronic inadequate sleep causes our physiological stress responses to be exaggerated in reaction to psychological stresses. That means that if we’re not getting enough good sleep, our adrenal glands kick into high gear more easily in response to things like deadlines, psychotic bosses, and traffic jams. The combination of chronic stress and poor sleep is a recipe for adrenal fatigue.
It’s no secret that I’m a huge advocate for sleep health in our modern, sleep-deprived world (have you seen my epic online program Go to Bed?). Sleep also inherently has a huge impact on our adrenal glands, because our circadian rhythm is regulated in part by the HPA axis and the biphasic effects of cortisol and melatonin (melatonin is the hormone that helps us to sleep at the end of the day, and it is not released when circulating levels of cortisol are too high). In fact, entrenching our circadian rhythm is one of the main mechanisms to improving the balance between cortisol and melatonin (see Regulating Circadian Rhythm (and why that’s important) and The Importance of Sleep).
But increasingly, research indicates links between sleep and stress that highlight the potential for a vicious cycle. Poor sleep makes us less resilient to stress and chronic stress wrecks our sleep quality (ever find yourself tossing and turning at night worried about bills or thinking about your To Do list?). While it may seem like this link makes it doubly hard to claw our way back to healthy adrenals, it actually highlights the possibility of managing stress by managing sleep (and managing sleep by managing stress).
There are a few simple strategies that can go a long way in terms of improving sleep quality. First and foremost is carving out enough time in our 24-hour days for sleep; we need 7 to 9 hours total sleep on average which typically means 7.5 to 10 hours in bed each night (see Sleep Requirements and Debt: How do you know how much sleep you need?). Importantly, even a small deficiency in sleep can have a pretty huge negative impact on our health (see Sleep and Disease Risk: Scarier than Zombies!). Second, is entrenching circadian rhythms by being mindful of important zeitgebers (see Regulating Circadian Rhythm (and why that’s important)) like the light-dark cycle, meaning we need exposure to bright (blue) light during the day, dim (red) light in the evening, and darkness while we’re sleeping. Of course, there’s a whole lot more we can do to improve sleep, mostly requiring only small adjustments to our choices. You can learn more about the relationship between sleep and cortisol, as well as dozens of strategies for improving sleep, in my online program Go to Bed.
 Meditate Regularly
Meditate Regularly
Meditation is one of the best-studied methods for increasing resilience to stress (yes, it sounds crunchy, but there’s actually a ton of science to support it!). This ancient method of mind-body medicine is calming practice that involves regulating one’s attention and/or systematically focusing on inner or outer experiences. It is generally performed seated or while resting, but walking meditation is also sometimes employed. Depending on the type of meditation used, a phrase (called a “mantra”) may be repeated internally or out loud. While some use meditation as a spiritual practice, but that is not necessary to reap the benefit! There are many different types of meditation, so I recommend exploring the many options before settling on a personal favorite (or quitting because meditation doesn’t feel right!).
Supplementation & Herbal Medicine
There are many supplements and herbal products marketed to people with adrenal fatigue, and they aren’t all good! There is a lot of misinformation about what these products are and how they may (or may not) be affecting our adrenal glands. Because supplement regimes for adrenal fatigue must be discussed with a healthcare provider and catered to each individual’s needs, this isn’t an exhaustive list; however, it’s a starting point for discussions with your healthcare professional.

General Adrenal Support
First, let’s review what specific supplementation may be best for overall adrenal support. Based on what we know of the metabolic demands on the adrenal glands,
- Omega 3 fatty acids, as I discussed earlier, are an essential aspect of any anti-inflammatory protocol. There are a lot of supplements of both whole food and not-whole-food origin that purport to be high in omega-3s, so it’s worth discussing the details of which omega-3s we would want: EPA and DHA. These are end-product members of the omega-3 fatty acid family that are readily usable in the body; in contrast, ALA (which is high in seed oils like flax and chia) has a very low conversion rate and is thus less bioavailable. So, going for supplements that are high EPA and DHA is best for an omega-3 fatty acid boost. Of course, whole foods sources are even better since polyunsaturated fats oxidize much less readily while still part of the matrix of a whole food. My favorite source of omega-3s is organ meats and fatty coldwater fish like salmon.
- Vitamin C is a nutrient that is tied very closely with adrenal function. The adrenal glands are actually one of the only sites in the body where vitamin C is stored in any appreciable amount. Part of the reason for this is that vitamin C is used in the production of hormones for both the HPA and HPG axes, including cortisol. In states of stress, vitamin C stores are depleted (this is one of the reasons that we see such a huge decline in immune system function when someone struggles with adrenal fatigue).
- Riboflavin (Vitamin B2) deficiency is linked with adrenal function, and we know that the use of riboflavin to make cellular energy molecules (like FAD and FMN) is impaired in people with adrenal insufficiency and hypothyroidism. Making sure to get enough vitamin B2 could support our adrenals through times of stress or if we are worried about adrenal fatigue.
- Pantothenic Acid (Vitamin B5) is an essential vitamin used in the production of sex and stress hormones (aka cortisol), so making sure that we’re sufficient in our vitamin B5 is a good way to support our adrenal glands. This vitamin is included in pretty much any and all multivitamin or B vitamin complex, and it is rare for us to have a deficiency, but targeted support may be necessary if we are acutely stressed and need to make tons of cortisol.
- Cobalamin (Vitamin B12) is another source of potential adrenal support for both prevention and treatment of HPA axis dysregulation. It is hypothesized that vitamin B12 acts as a metabolic buffer for the effects of cortisol, so the physiological effects of stress are better contained, making our bodies more robust during times of stress.
Specialized Adrenal Support
- Desiccated adrenal gland (adrenal cortex) is a popular supplement suggested for people with adrenal fatigue. This supplement is made from dried animal adrenal glands is believed to support our human adrenals, though it’s hard to know exactly what is included in these kinds of supplements (from a nutrient perspective and otherwise).
- Pregnenolone supplementation is used when someone is suspected to be experiencing pregnenolone steal (which we discussed in Part 1). The signs of pregnenolone steal generally include changes in both stress response (HPA axis dysregulation) and sex hormone-related issues like changes in menses (HPG axis dysregulation). Making pregnenolone more available for both biochemical pathways by taking it orally could alleviate some of these symptoms. However, one should never take hormones or hormone precursors without consulting a medical practitioner.
Herbal Support & Adaptogenic Herbs
Adaptogenic herbs are the most commonly used type of herb in response to chronic stress or adrenal fatigue. In medical herbalist communities, adaptogenic herbs used for their “normalizing” effect on our physiology, helping to make us more resistant to stressors; so, they are believed to lower cortisol output in phase 2 and increase cortisol output in phase 3. But, within the spectrum of adaptogenic herbs, some are considered to be more stimulating (like the gingsengs) and others are more relaxing (like ashwagandha) and yet others support adrenal health generally (are neither stimulating nor relaxing). That’s important, because if you want to choose adaptogens based on exactly what your cortisol is doing throughtout the day (deteremined by test results; see Demystifying Adrenal Fatigue, Pt. 2: Testing Adrenal Glandular Function), namely you want to suppress cortisol production when its too high and stimulate it when its too low. This can mean taking different adaptogens at different times of day. Many popular herbal formulas include both stimulating and relaxing adaptogenic herbs and non-adaptogenic herbs, so pay careful attention to the ingredients these products (which might be in the form of a tea, tincture, tonic, or pill) and which specific herbs they contain!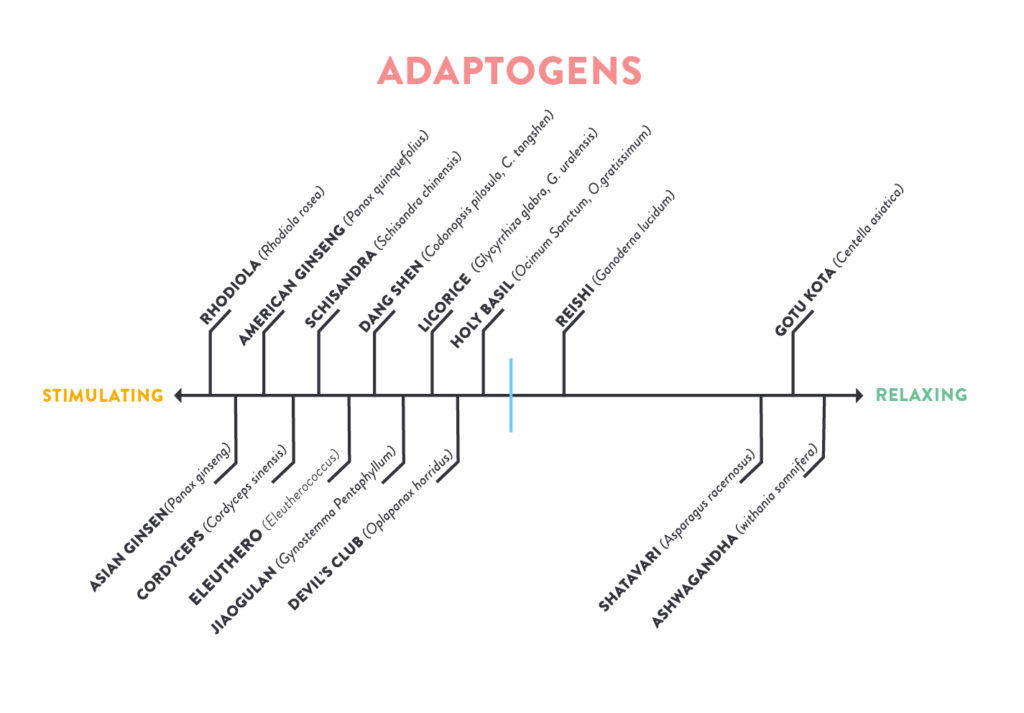
 Here is a review of some of the most popular, well-studied adaptogenic herbs:
Here is a review of some of the most popular, well-studied adaptogenic herbs:
- Ashwagandha (Withania somnifera) is probably the best-known adaptogenic herb that is often used in the treatment of adrenal fatigue. This herb has strong adaptogenic properties and is also immunomodulating, so it combats some of the effects of stage 2 and 3 adrenal fatigue as well. Plus, it is known to have anti-anxiety and –depression effects, so it helps with the mood issues associated with adrenal fatigue as well. Ashwagandha is considered the most relaxing herb on the spectrum of adaptogens.
- Licorice Root (Glycyrrhiza) is another adaptogenic herb oftentimes used in adrenal fatigue preparations. However, because of its stimulating nature, this herb is not a good fit for people with too much cortisol.
- Gotu kola is a traditional adaptogen that is also more relaxing than stimulating. This herb may also have some cognitive benefits.
 Siberian ginseng (Eleutheroccocus senticosis) is used to increase resistance to infection and stress, improve physical performance, and improve mood.
Siberian ginseng (Eleutheroccocus senticosis) is used to increase resistance to infection and stress, improve physical performance, and improve mood.- Asian ginseng (Panax ginseng) is an adaptogenic herb that has stimulating properties, so it is best used during stage 3 adrenal fatigue to help support more cortisol production.
- American ginseng (Panax quinquifolium) is another species of ginseng that is more purely adaptogenic with mild stimulating properties. Research has shown that long term administration (3-6 months) is necessary to see any effects, so this herb is used more in support of other primary herbs.
 Golden Root (Rhodiola rosea) is an adaptogen that decreases fatigue and helps with endurance, so it is best in a stage 1 situation (where we’re dealing with a lot of stress).
Golden Root (Rhodiola rosea) is an adaptogen that decreases fatigue and helps with endurance, so it is best in a stage 1 situation (where we’re dealing with a lot of stress).
Believe it or not, this is only a short list of all the adaptogenic herbs available to us – and there are even more that aren’t specifically adaptogenic that may be used in combination. When using herbal products, work with a trained practitioner who knows the pros, cons, and interactions of each of these herbs and others!
Conclusions
Adrenal fatigue and supporting adrenal gland function is a hot topic in the complementary and alternative medicine community right now. In this series of blog posts, we have discussed the details of what adrenal fatigue is, how to test for it, and some methods for gentle and effective adrenal support. While there are many specific methods that are used to diagnose and treat adrenal fatigue, there are simple and evidence-based ways that we can all support these incredibly important glands (and all the hormones they produce!).
Citations
Bassett SM et al. Sleep quality but not sleep quantity effects on cortisol responses to acute psychosocial stress. Stress. 2015;18(6):638-44
Head KA, Kelly GS. Nutrients and botanicals for treatment of stress: adrenal fatigue, neurotransmitter imbalance, anxiety, and restless sleep. Altern Med Rev. 2009;14(2):114-40.
Lane JD et al. “Caffeine affects cardiovascular and neuroendocrine activation at work and home”. Psychosom Med. 2002 Jul-Aug;64(4):595-603.
Lane, J.D et. Al. “Caffeine effects on cardiovascular and neuroendocrine responses to acute psychosocial stress and their relationship to level of habitual caffeine consumption. Psychosomatic Medicine”. 1990. 52(3):320-36.
Lovallo WR et al. “Stress-like adrenocorticotropin responses to caffeine in young healthy men” Pharmacol Biochem Behav 1996;55:365–9.
Lovallo, W. et. a. “Caffeine Stimulation of Cortisol Secretion Across the Waking Hours in Relation to Caffeine Intake Levels”. Psychosomatic Medicine. 2005. 67:734-739
Zampelas A et al. “Associations between coffee consumption and inflammatory markers in healthy persons: the ATTICA study”. Am J Clin Nutr. 2004 Oct;80(4):862-7.




 TPV Podcast Episode 226, The Perfect Plate?
TPV Podcast Episode 226, The Perfect Plate?