The first paper from Dr. Terry Wahl’s clinical trials, titled “A Multimodal Intervention for Patients with Secondary Progressive Multiple Sclerosis: Feasibility and Effect on Fatigue“, has been e-published ahead of print in the Journal of Alternative and Complementary Medicine. And this is exciting news!
The recommendations in The Paleo Approach are compiled from insights gleaned from over 1200 scientific studies. Each of these studies provided guidance for one tiny piece of the puzzle. For example, one study would show that vitamin D deficiency is correlated with autoimmune disease. Another study would show that fish oil supplementation reduces symptoms of autoimmune disease. Yet another study shows that wheat germ agglutinin stimulates the immune system. I took all these tiny pieces and wove together a set of recommendations aimed at regulating the immune system, regulating hormone systems, restoring gut barrier function, and nurturing a healthy ecosystem for our gut bacteria to thrive in. I know from personal experience and from thousands of others that this works. I can point to scientific papers that explain why (at least for each individual tiny piece). But all this is still anecdotal. What has been missing is the clinical trials to prove the effectiveness of a nutrient-dense Paleo diet to reduce autoimmune disease symptoms. Until now.
The first paper from Dr. Terry Wahls’ clinical trials is about to be published (unfortunately, the article is only available as an e-publication ahead of print to subscribers of the Journal of Alternative and Complementary Medicine; the rest of us have to pay to read it). Not familiar with Dr. Wahls? Dr. Wahls is both an inspiring testament of the power of nutrition herself and is contributing to the scientific literature on the role of diet in disease by running the first clinical trials evaluating the effectiveness of a nutrient-dense Paleo diet for the management of autoimmune disease, in his case secondary-progressive multiple sclerosis. She is also the author of a fantastic new book, The Wahls Protocol, which I highly recommend.
Dr. Wahls’ clinical trials are directly inspired by her own personal battle with secondary-progressive multiple sclerosis (I recommend watching the viral YouTube video of her TedX-IowaCity talk from fall 2011). She found something that worked, that reduced her symptoms and seemingly reversed her disease . And now she is testing whether or not this approach can work for other people suffering from MS through methodical clinical trials. And the early results show that it can.
So, on to the paper:
The initial trial was focused on safety and compliance. It was a small study, only 10 subjects who were followed for a year. The study included exercise, meditation, neuromuscular electric stimulation (NMES), supplements and diet changes. The diet changes were focused on eating 9 cups of vegetables per day (3 cups each of green veggies, colorful veggies, and sulfur-rich veggies), animal and fish protein and encouraged fish oil consumption, nutritional yeast consumption, kelp and algae consumption, allowed non-dairy milk substitutes, limited non-gluten containing grains, and completely eliminated dairy, gluten, and eggs. These interventions were modelled after what Dr. Wahls did personally to reduce the symptoms of her disease. Because the trial was based on Dr. Wahls as a preliminary experiment, they were not allowed to deviate for this initial trial.
One of the most important results of this study is that compliance with the diet changes was high (interestingly, compliance with the supplements was low and the subjects were not required to take the supplements if they did not want to). What does compliance mean? That means how close what the person ate matched the recommendations. In the pharmaceutical industry, compliance is used to measure how well a drug works versus how bad the side effects are. If the drug works wonders and there’s no side effect, people tend to keep taking it. If the drug doesn’t do much and the side effects are unbearable, people tend to stop taking it. When you’re asking people to make huge changes to their diet, compliance is a great measure of how much improvement those people are seeing from those diet changes. And it gives you some indication about how realistic it is to include diet recommendations that are a huge departure from what people more typically eat as part of a disease management strategy. Due to copyright issues, I can’t show you the graphs from the paper, but I can show you these two:
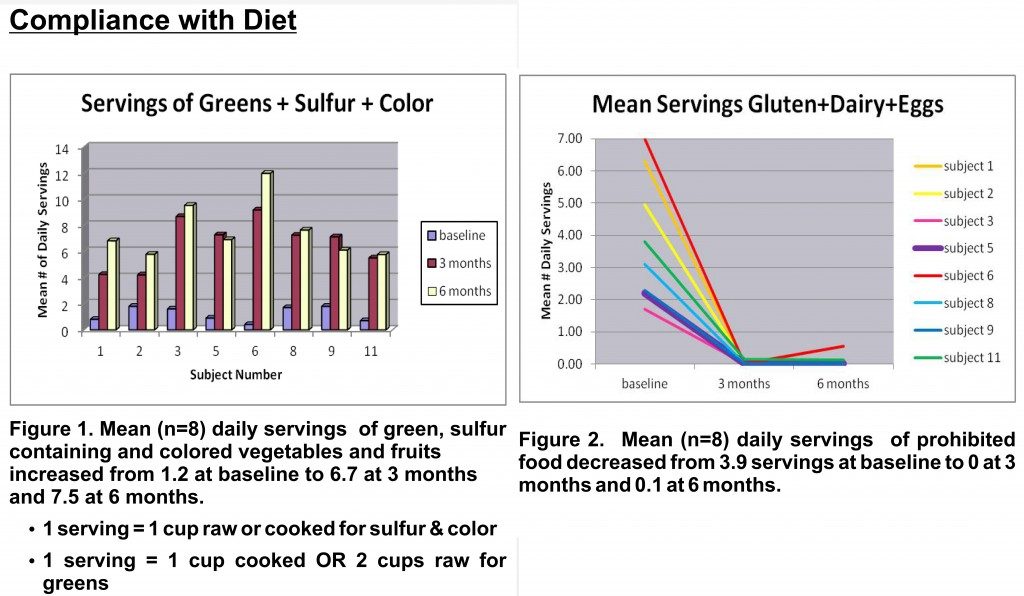
These graphs are from before the clinical trial ended, so there’s only data from the first six months. The subjects on average were eating five or six times more vegetables than they were before the trial. And the subjects gave up gluten, dairy and eggs successfully. The subjects did even better at 12 months.
For those firmly entrenched in the Paleo community, compliance with these diet changes might not seem like such a big deal. We’ve all chosen to eat this way. But, let me remind you about the beginning. About transition. About not wanting to give up favorite foods. And the subjects in this clinical trial weren’t in search of elite fitness or weight loss, they were just people struggling with advancing multiple sclerosis who were ready to try something new. This is really cool.
Now on to how this impacted the patients. The primary outcome measured in this first paper was fatigue. All subjects showed marked improvements in perceived fatigue over 12 months. Due to copyright issues, I can’t show you the graph from the paper, but I can show you this one.
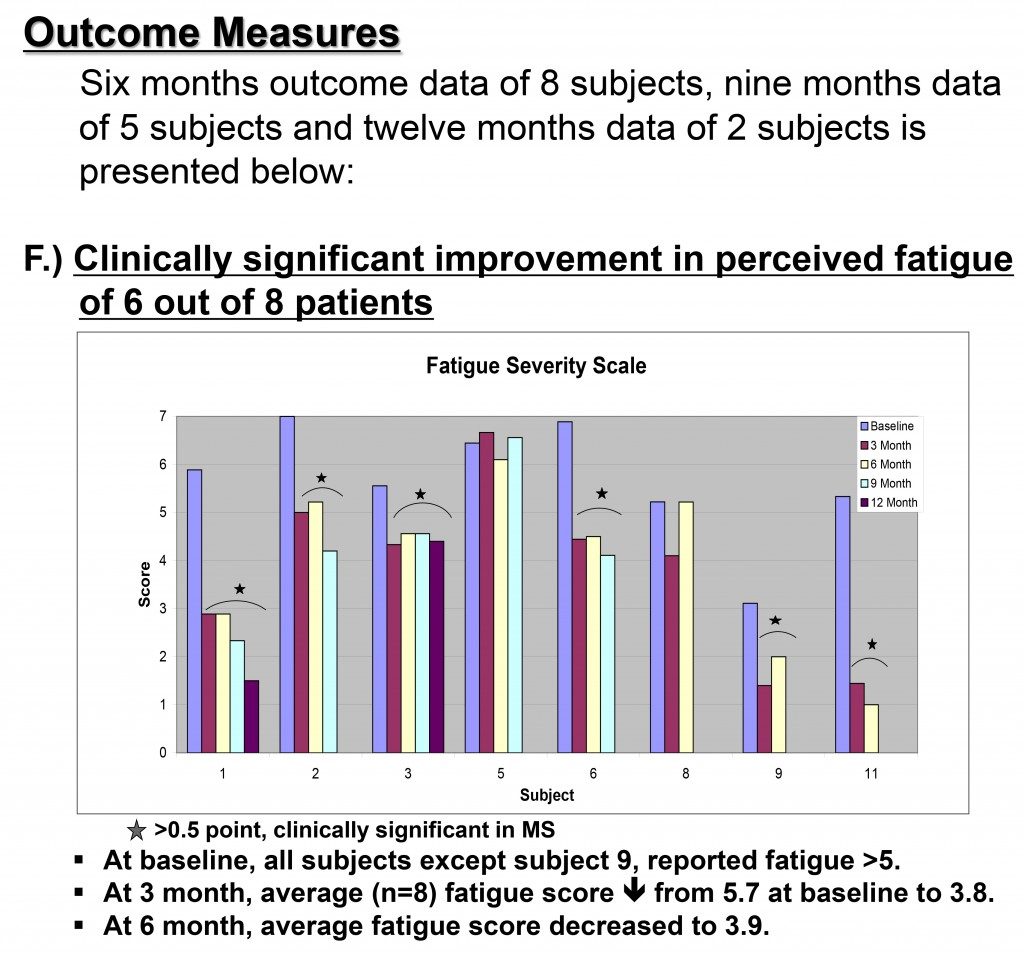
Again, this is from preliminary data. Every patient reported having less fatigue. And the results are even more impressive at 12 months. And this is pretty fantastic. And if you’re suffering from the debilitating fatigue that goes with MS, you’re probably looking at this and are ready to jump in with both feet.
Save 70% Off the AIP Lecture Series!
Learn everything you need to know about the Autoimmune Protocol to regain your health!
I am loving this AIP course and all the information I am receiving. The amount of work you have put into this is amazing and greatly, GREATLY, appreciated. Thank you so much. Taking this course gives me the knowledge I need to understand why my body is doing what it is doing and reinforces my determination to continue along this dietary path to heal it. Invaluable!
Carmen Maier

Even more exciting is where these clinical trials are ongoing. More patients have been enrolled and followed (now for two years). More measurements have been made. Now, Dr. Wahls is working on teasing out the effects from the diet separately from the other interventions in this initial clinical trial. Now, there’s randomization and comparisons against the standard American diet. And the early results from these measures in the ongoing trials are even more exciting.
The ongoing clinical trials are showing improvement in a variety of markers of health: C-reactive protein (a blood marker of inflammation), serum homocysteine (which is high when the liver and kidneys aren’t functioning properly), blood triglycerides, pain, walking speed, and a variety of other measures. The studies are also showing mental health improvements. MS sufferers have more hope for the future after following the Wahls Protocol
Dr. Wahls’ preliminary research into the intersection of nutrition and health was focused on mitochondrial health (her first book is called Minding my Mitochondria). Mitochondria are the energy factories within every cell of our bodies. When the mitochondria are starved of the nutrients they need to function properly, every cell in the body suffers. What’s interesting is that Dr Wahls’ conclusions are nearly identical to mine although I come at these recommendations by examining the function and regulation of the immune system (we both recommend diets high in organ meat, seafood, tons of veggies, high quality meats, some fruit–because of the micronutrient content of these foods). The ongoing clinical trials have a focus on gluten-free, dairy-free, and high vegetable consumption as detailed above. However, Dr. Wahl’s is currently recruiting for a new clinical trial that is going to be even more sophisticated, comparing this simpler diet from the initial trials with what Dr. Wahls calls the Wahls Protocol Plus, which is virtually identical to The Paleo Approach. I am even more excited to see the results from this one!
Dr. Wahls is actively recruiting for her latest clinical trial. If you or someone you know has MS, please see this page for more information including eligibility criteria.
Both Dr. Wahls and I are passionate about nutrient-density. We both believe that a lack of sufficient dietary vitamins, minerals, and other micronutrients like Coenzyme Q10 and phytochemicals are major contributors to all chronic diseases. So, one of the things that Dr. Wahls is doing with her clinical trials is analyzing the micronutrient content of the subject’s diets. Here’s some preliminary research from that part of the trial.
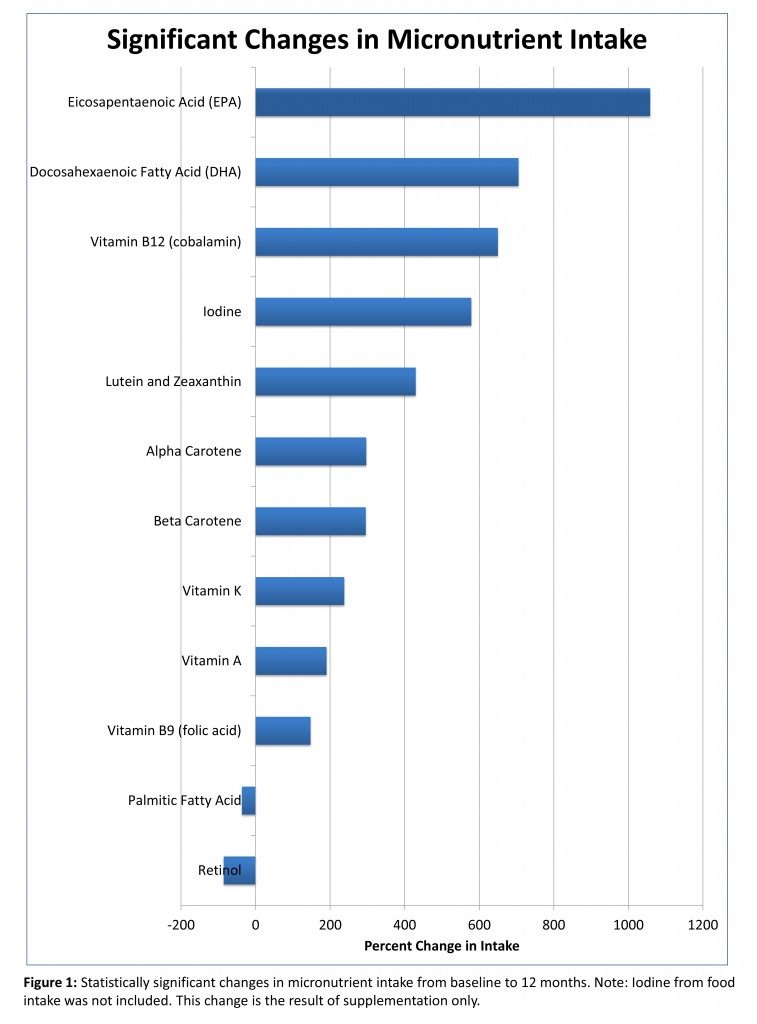
Dr. Wahls’ contribution to science is vital. She is drawing attention to the importance of diet (and lifestyle with her exercise and meditation interventions) in managing autoimmune disease. She is providing authenticity to what so many thousands of people have experienced already by experimenting on themselves.
So, what about other autoimmune diseases? Prof. Loren Cordain is also working on a scientific paper showing that a Paleo diet has a therapeutic effect in autoimmune thyroid diseases and Crohn’s disease. When this paper is published, you can bet I’ll also be sharing it with you too!
 I want to thank Dr. Terry Wahls for sharing her research groups posters and preliminary data with me and giving me permission to share her exciting research with you. The Wahls Protocol is available for pre-order now and will be released March 13th, 2014. It’s a perfect companion to The Paleo Approach, is an engaging and informative read, and I highly recommend it. I would also like to thank Prof. Loren Cordain for sharing his preliminary research with me.
I want to thank Dr. Terry Wahls for sharing her research groups posters and preliminary data with me and giving me permission to share her exciting research with you. The Wahls Protocol is available for pre-order now and will be released March 13th, 2014. It’s a perfect companion to The Paleo Approach, is an engaging and informative read, and I highly recommend it. I would also like to thank Prof. Loren Cordain for sharing his preliminary research with me.





 50/50/50 Burgers
50/50/50 Burgers